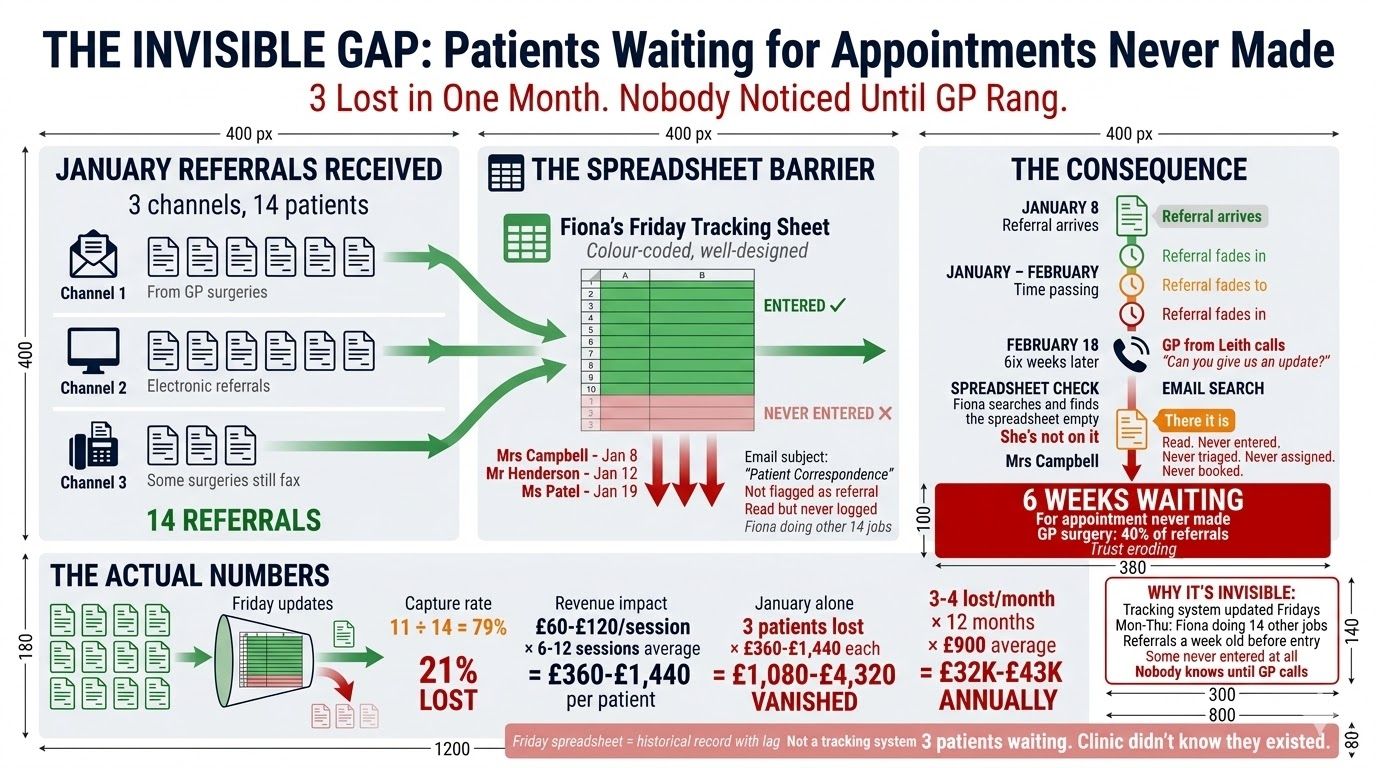
TL;DR: A multi-practitioner physio clinic in Edinburgh was tracking referrals in a colour-coded spreadsheet that the practice manager updated on Fridays. Referrals arrived through three channels: email, NHS SCI Gateway, and fax. Three of fourteen January referrals were never entered. One patient waited six weeks before her GP rang asking for an update. We built a five-stage referral tracking agent that captures every referral the moment it arrives, triages by urgency, assigns to the right practitioner, tracks milestones through to discharge, and auto-generates NHS Scotland reports. Lost referrals dropped to zero. Time from referral to first appointment: 8.2 days down to 3.1. Fiona's admin time: 10+ hours per week down to 2. The referring GP surgery increased referrals by 15%. Agent cost: £140/month.
The Call from Leith
February. A GP surgery in Leith rings the clinic. "We referred a patient to you six weeks ago. Mrs Campbell. Knee pain, post-surgical rehab. Can you give us an update?"
Fiona, the practice manager, checks the spreadsheet. Mrs Campbell isn't on it.
She checks the email inbox. There it is. A referral letter from January 8th. Read. Never entered into the spreadsheet. Never triaged. Never assigned to a practitioner. Never booked.
Mrs Campbell had been waiting six weeks for an appointment that was never made.
Fiona's stomach dropped. Not because this was unusual. Because she knew there were probably more.
She went through January's referrals against the spreadsheet. Fourteen received across all channels. Eleven entered. Three missing.
Three patients. Waiting for a clinic that didn't know they existed.
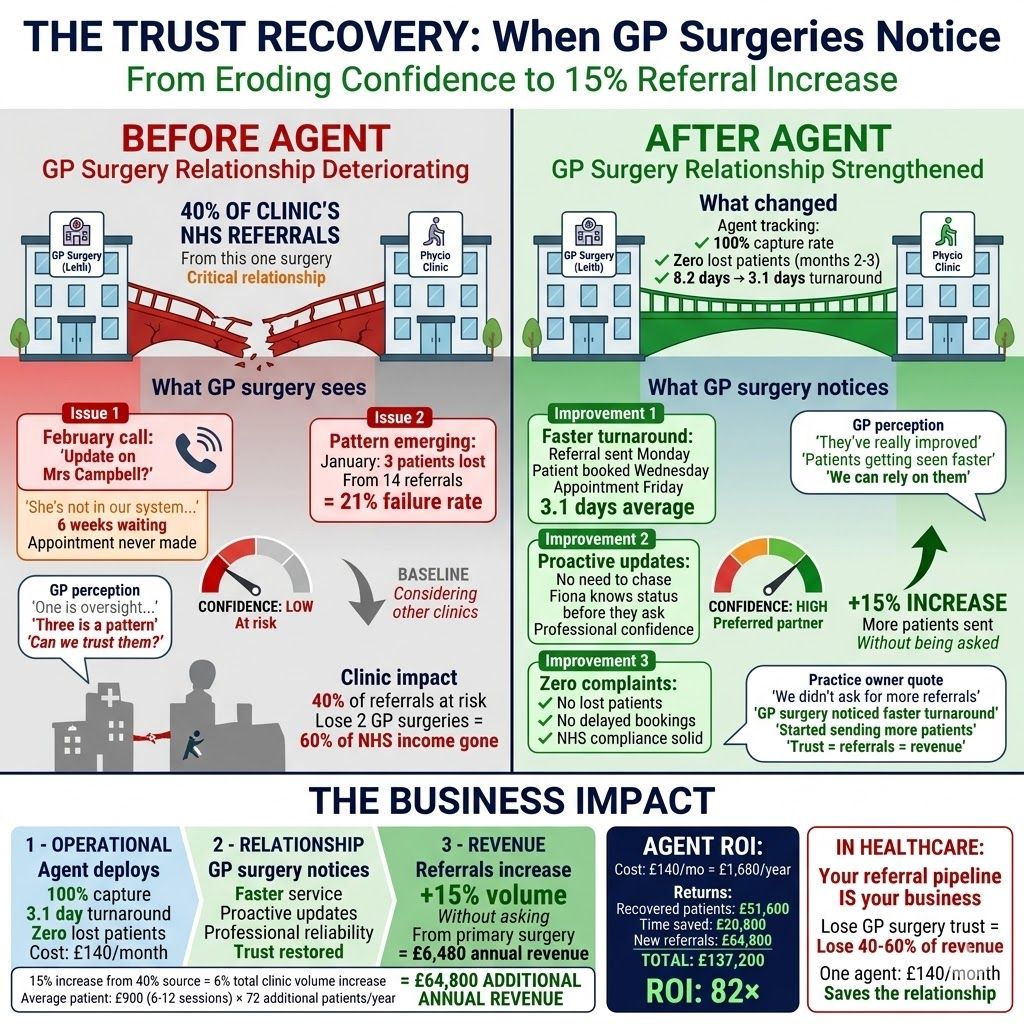
The GP on the phone was polite about it. But Fiona could hear the note underneath. This surgery accounted for 40% of the clinic's NHS referrals. One lost patient is an oversight. Three in one month starts to look like a pattern.
"I'll get Mrs Campbell booked in today," Fiona said. And she did. But the question she couldn't shake was how many other months had looked like January without anyone noticing.
The Clinic
Multi-practitioner physiotherapy practice in Edinburgh, Scotland. Four physios, Fiona as practice manager, and one receptionist. A mix of NHS-referred patients and private self-referrals. Thirty to forty new referrals per month.
Referrals arrive through three channels. Email from GP surgeries. The NHS SCI Gateway system for electronic referrals. And occasional fax, because some surgeries in the Lothians haven't fully transitioned to digital. Three channels, one person responsible for checking all of them.
Fiona's job title is practice manager. Her actual job is everything that isn't treating patients. Referral intake, scheduling, billing, NHS reporting, practitioner rotas, reception cover, supplier orders, insurance queries. Roughly 15 distinct responsibilities. Referral tracking is one of them.
Her tracking system: a colour-coded spreadsheet she updates on Fridays. Green for booked, yellow for pending, red for overdue. Monday to Thursday, she's doing the other 14 jobs. By Friday, some referrals are a week old before they're entered. Some, as January showed, don't get entered at all.
The revenue maths: each missed referral represents £60 to £120 per session across an average course of six to twelve sessions. That's £360 to £1,440 per patient. Three lost patients in January alone was somewhere between £1,080 and £4,320 in revenue that simply vanished. Not because anyone said no. Because nobody said anything at all.
And then there's NHS Scotland reporting. Monthly data submissions on referral-to-treatment times, waiting list statistics, patient outcomes. Fiona compiles these manually, cross-referencing the spreadsheet with the appointment system. Two-plus hours every month, and she knows the numbers are only as good as the spreadsheet.
Why Nothing Had Worked
The spreadsheet was well-designed. Colour-coded, structured, clear. The problem wasn't the spreadsheet. It was that it only reflected reality when Fiona had time to update it. A tracking system that's current four days out of seven isn't a tracking system. It's a historical record with a lag.
Their practice management software handled appointments and billing but had no referral pipeline tracking. It knew Mrs Campbell existed once she had an appointment. It had no idea she existed between the referral arriving and someone booking her in. Upgrading to a system with pipeline tracking meant £400-plus per month and a data migration nobody could face during busy periods.
Fiona created a "Referrals" folder in the shared email inbox. But referrals arrived mixed with appointment queries, patient communications, and supplier emails. The January email about Mrs Campbell had the subject line "Patient Correspondence — Dr Murray." Not "Referral." It got read and lost.
NHS SCI Gateway covered electronic referrals, but only a portion of the clinic's intake came through it. Some GPs still emailed. A few still faxed. And the Gateway tracked whether the referral was sent, not whether the clinic acted on it.
Every fix depended on Fiona having time she didn't have.
What We Built
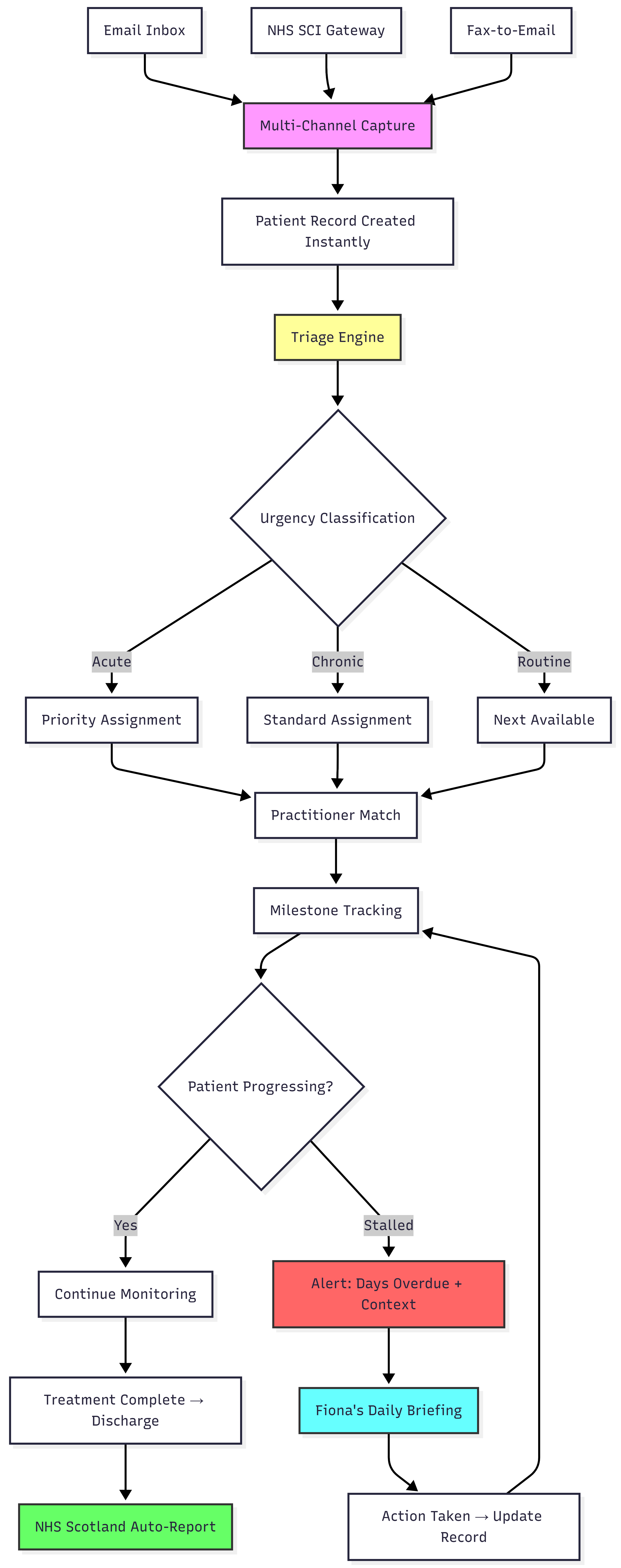
Five stages, running continuously across all three intake channels.
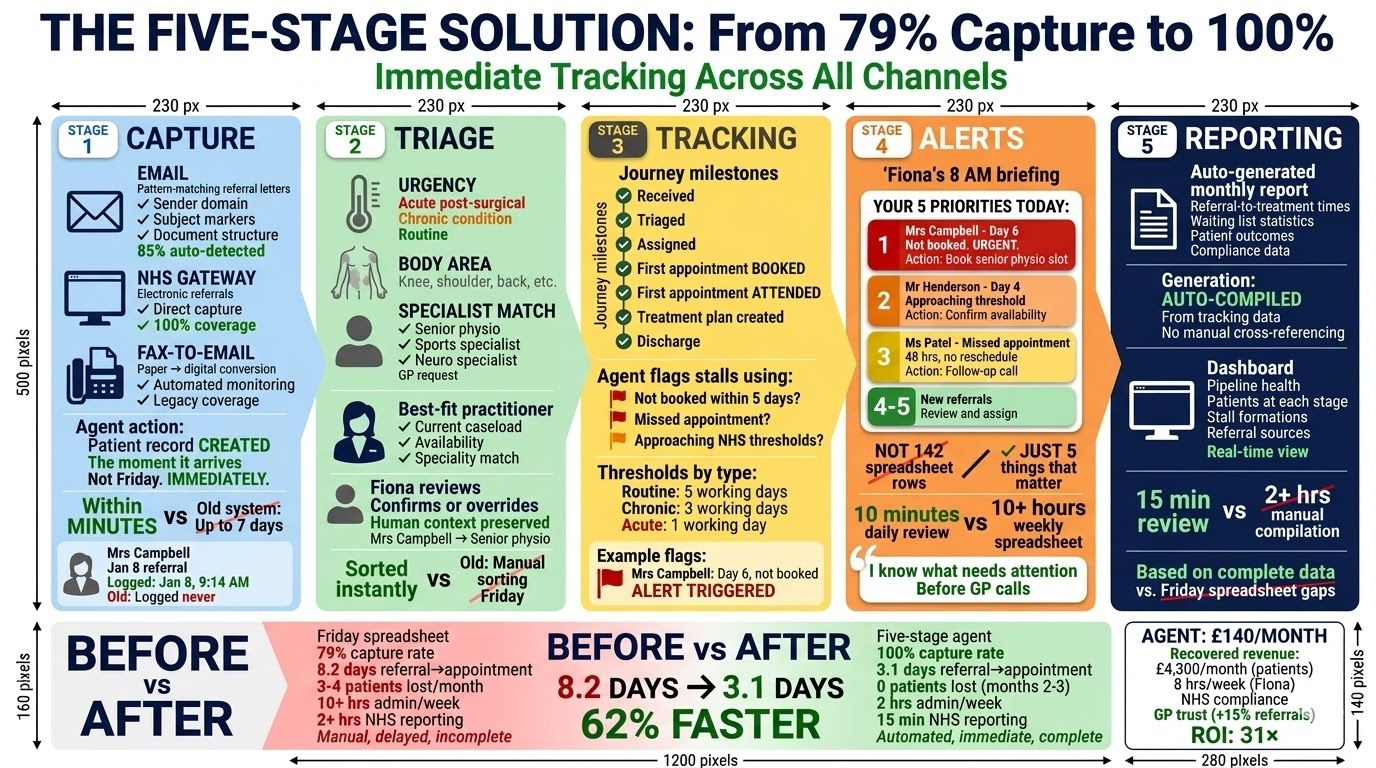
Stage 1: Multi-channel referral capture
The agent monitors all three channels. It pattern-matches referral letters in the email inbox, distinguishing them from general correspondence by sender domain, subject line markers, and document structure. It connects to the NHS SCI Gateway API for electronic referrals. And it monitors a fax-to-email service that converts the remaining paper referrals into digital records.
The moment a referral arrives through any channel, a patient tracking record is created. Not on Friday. Not when someone has time. Immediately.
This is the step that would've caught Mrs Campbell. Her referral letter arrived on January 8th. Under the old system, it sat in an inbox until Fiona got to it. Under this system, it would've been logged within minutes.
Stage 2: Triage and assignment
Each referral gets categorised by urgency (acute post-surgical, chronic condition, routine), body area, and any practitioner specialisms noted in the referral. The agent suggests assignment to the best-fit physio based on speciality, current caseload, and availability. Fiona reviews and confirms or overrides. She knows Mrs Campbell's GP asked for the senior physio because of the post-surgical complexity. That context still needs a human. The sorting doesn't.
Stage 3: Milestone tracking
Every patient gets monitored through the referral journey: received, triaged, assigned, first appointment booked, first appointment attended, treatment plan created, discharge. The agent flags patients who stall at any stage beyond expected timeframes.
A patient who hasn't been booked for a first appointment within five working days of referral gets flagged automatically. A patient who missed their first appointment without rescheduling gets flagged at 48 hours. A patient approaching NHS waiting time thresholds gets flagged with enough lead time for the clinic to act.
Stage 4: Proactive alerts
Fiona gets a daily morning summary at 8 AM. New referrals received since yesterday. Patients approaching threshold deadlines. Patients overdue at any milestone. Not 142 rows in a spreadsheet. Five things that need attention today, with context on why each one matters.
This was the design choice that changed Fiona's relationship with referral tracking. Instead of dreading Friday's batch update, she spends ten minutes each morning reviewing the briefing and handling exceptions. The cognitive load dropped dramatically.
Stage 5: NHS reporting and dashboard
The monthly NHS Scotland data submission generates automatically from the tracking data. Referral-to-treatment times, waiting list stats, patient outcomes. Fiona reviews and submits. What took two-plus hours of manual compilation now takes fifteen minutes of review.
A practice-wide dashboard shows pipeline health at a glance. Patients at each stage. Where stalls are forming. Which referral sources are most active.
What We Learned Building It
Healthcare data sensitivity added a layer. Patient data in Scotland falls under UK GDPR and NHS Scotland's information governance standards. The agent processes referral data but doesn't store patient records outside the clinic's existing systems. It creates tracking entries with patient identifiers that link back to the practice management system. We spent a week on the data architecture to make sure nothing patient-identifiable lived anywhere it shouldn't. Worth the time. Non-negotiable in healthcare.
Email pattern-matching needed training. GP surgeries don't use standardised referral formats. Some send structured forms. Some send a PDF attachment with "please see attached" in the body. Some write details directly in the email. Dr Murray's email about Mrs Campbell had the subject "Patient Correspondence," which is exactly why it was missed. We built pattern-matching rules for the twelve most frequent referring surgeries, covering about 85% of email referrals. The remaining 15% get flagged as "possible referral — please confirm," which Fiona handles in her morning briefing.
The five-day booking threshold was controversial. The physios initially pushed back. "Some patients need specialist slots that aren't available within five days." Fair point. We built flexibility: standard threshold of five working days for routine, three for chronic, and one for acute post-surgical. Each can be overridden with a reason that gets logged. The override rate in the first quarter was about 12%, mostly for specialist slots. That's healthy. It means the threshold is tight enough to catch genuine delays but not so rigid it creates false urgency.
Fiona cried on day three. Not from frustration. From relief. She said she'd been carrying the mental weight of "what am I missing?" for four years. The morning briefing meant she started each day knowing exactly what needed attention, instead of wondering what she'd forgotten. That's not a metric. But it's real.
The Numbers
Metric | Before | After |
|---|---|---|
Referrals captured at intake | ~79% | 100% |
Time from referral to first appointment | 8.2 days | 3.1 days |
Patients lost between referral and first appointment | 3-4/month | 0 (months 2-3) |
Fiona's referral admin time/week | 10+ hrs | 2 hrs |
NHS reporting time/month | 2+ hrs manual | 15 min review |
GP referral volume (primary surgery) | Baseline | +15% |
Agent cost/month | N/A | £140 |
The revenue maths: £140 per month for the agent against a conservative £4,300 per month in recovered patient revenue. Plus eight hours per week of Fiona's time back. Plus NHS compliance based on complete data instead of a Friday spreadsheet.
But the number the practice owner kept coming back to was the 15% referral increase from their primary GP surgery. He hadn't asked for it. It happened because the surgery noticed faster turnaround and started getting proactive status updates. In healthcare, your referral pipeline is your business. Lose the trust of two GP surgeries and you lose 60% of your NHS income.
The Pattern
If you're running a multi-practitioner healthcare practice and your referral tracking depends on one person updating a spreadsheet when they have time, patients are falling through cracks you can't see.
This isn't a healthcare-specific problem. It's a pipeline problem. Referrals are leads. Milestones are pipeline stages. Lost patients are lost revenue. The language changes by industry. The maths doesn't.
The agent doesn't replace Fiona's clinical knowledge or her relationships with the GP surgeries. It replaces the manual capture, tracking, chasing, and reporting that consumed ten hours of her week. Fiona still makes every clinical judgment. She still picks up the phone when a GP has a question. The agent makes sure she knows which questions are coming before they're asked.
At £140 per month, it's less than the revenue from a single lost patient's treatment course. The question isn't whether a practice this size can afford it. It's how many Mrs Campbells are sitting in an inbox right now, waiting.
Want to see if your practice has a similar referral gap? The AI Bottleneck Audit takes 5 minutes and shows you where patients or clients are disappearing. No pitch.
Want to see 25 agent architectures across different industries? Download Unstuck. It includes blueprints for intake, pipeline tracking, conflicts, engagement letters, and more.
by TR
for the AdAI Ed. Team